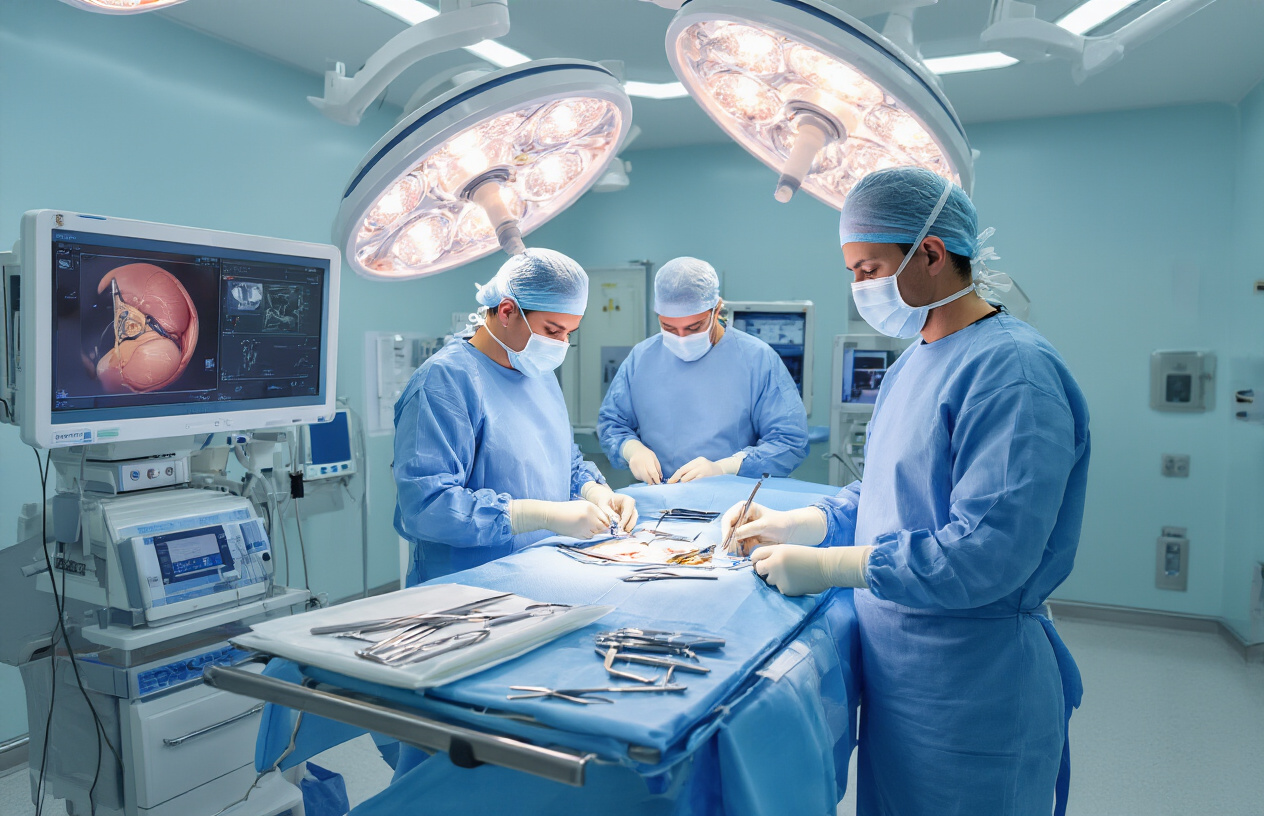
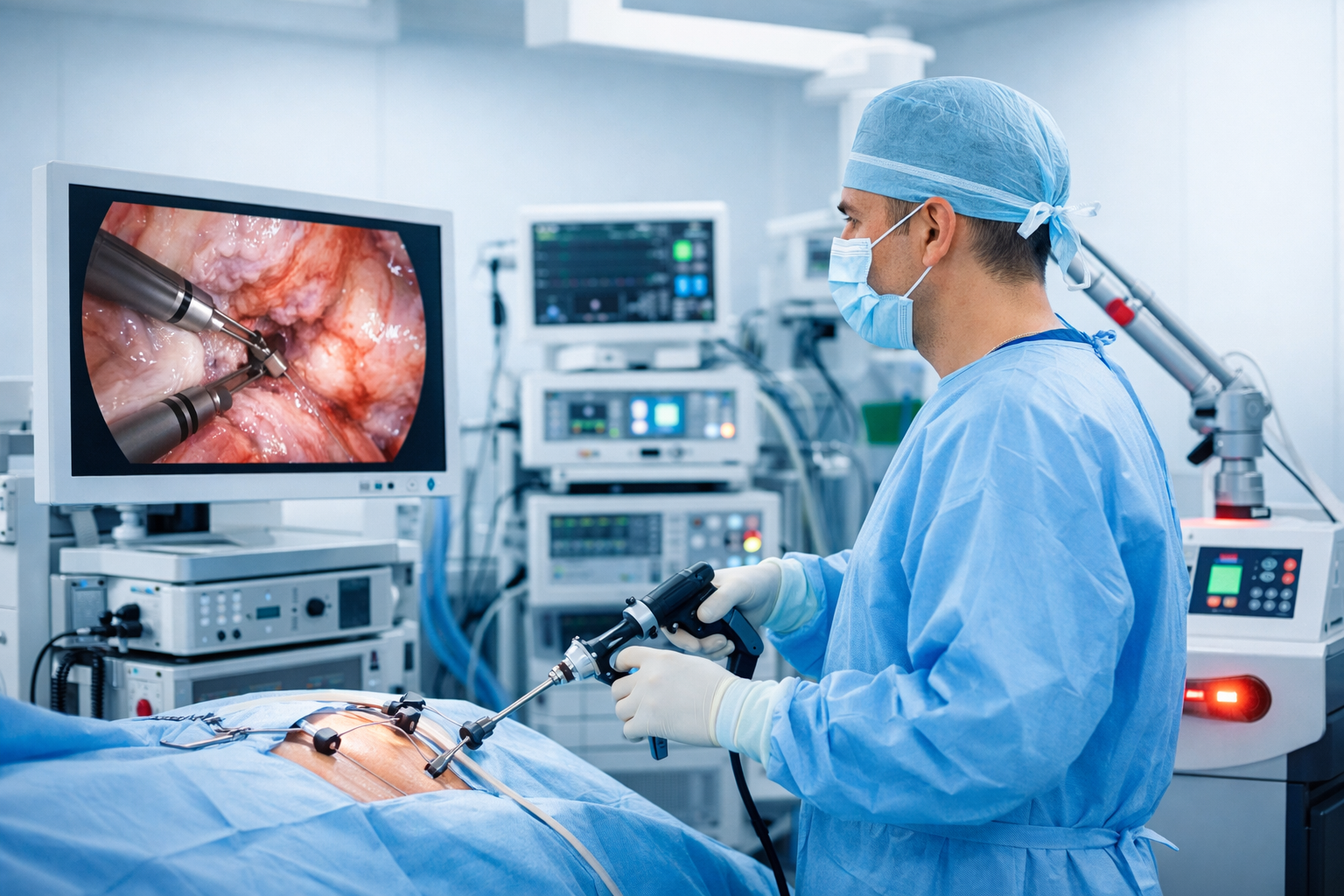
Here is a clear, step-by-step explanation of what typically occurs during laparoscopic surgery and laser surgery. Understanding each stage of this minimally invasive surgery helps patients feel more comfortable, informed, and confident before undergoing treatment.
1. Step-by-step procedure walkthrough
Your surgical experience begins well before you enter the operating theatre. After completing the necessary pre-operative evaluations and fasting instructions, you will be received by the surgical team who will confirm your identity and review the planned procedure. An intravenous (IV) line is then placed to administer medications and fluids, followed by general anesthesia to ensure complete comfort throughout the laparoscopic surgery.
Once anesthesia takes effect, the surgical team carefully positions you to provide the laparoscopic surgeon with optimal access to the treatment area. Small incisions, usually between 0.5 and 1.5 centimeters, are made in specific locations. These small openings allow specialized surgical instruments and the laparoscope—a thin, flexible tube with a high-definition camera—to enter the body.
Carbon dioxide gas is gently introduced into the abdominal cavity to create a working space by separating internal organs and tissues. This process, called pneumoperitoneum, allows surgeons to clearly view the internal structures while safely performing minimally invasive surgery.
The laparoscope sends real-time, magnified images to high-resolution monitors, giving the surgeon a detailed view of the surgical field. Laser surgery technology may be used for highly precise tissue cutting, coagulation, and removal of abnormal tissue. The focused laser energy produces clean incisions while sealing blood vessels simultaneously, helping reduce bleeding and minimizing trauma to nearby tissues.
During the procedure, surgical instruments are carefully guided through the small incisions to perform the required surgical steps. Whether the goal is removing diseased tissue, repairing an organ, or treating a specific condition, each movement is controlled and precise. After the surgical objectives are completed, the instruments are removed, the carbon dioxide gas is released, and the tiny incisions are closed using surgical adhesive or very small sutures.
2. Advanced monitoring and safety protocols
Modern operating rooms designed for advanced surgical treatment are equipped with advanced monitoring systems that continuously track your vital signs. Heart rate, blood pressure, oxygen saturation, and breathing patterns are monitored using specialized equipment that provides real-time information to the anesthesia team.
Maintaining the patient’s body temperature is also important during surgery. Temperature regulation helps promote healing and reduces the possibility of complications. Warming blankets and heated IV fluids are commonly used to maintain a stable core temperature throughout the procedure.
Laser safety measures are strictly followed during laser surgery procedures. Surgical team members wear specialized eye protection, and fire-prevention precautions are carefully implemented. Laser equipment is calibrated and tested before every operation to ensure consistent performance and beam accuracy. Emergency shutdown systems are also readily available so that the laser can be stopped immediately if required.
Infection control is another key priority in the operating room. The surgical area is completely sterilized and covered with sterile drapes, and antibiotics may be administered when appropriate. The entire surgical team follows strict aseptic protocols, while modern air filtration systems remove airborne particles and maintain positive pressure in the operating room to minimize contamination.
3. Surgical team coordination and communication
A successful surgical procedure depends on a highly coordinated medical team. Your surgical team typically includes an experienced laparoscopic surgeon, surgical assistants, an anesthesiologist or nurse anesthetist, circulating nurses, and surgical technologists. Each member has clearly defined responsibilities that contribute to patient safety and successful outcomes.
Communication protocols ensure that all team members remain informed about the progress of the procedure and any changes in the patient’s condition. Standardized terminology and clear verbal confirmations help reduce the possibility of misunderstandings during critical moments. Before surgery begins, a “time-out” safety check is performed to verify the patient’s identity, confirm the surgical site, and review the planned treatment.
The surgeon leads the procedure and makes the key surgical decisions while collaborating with the team regarding positioning, instruments, and surgical technique. Meanwhile, anesthesia specialists focus on the patient’s comfort and physiological stability, adjusting medications and monitoring vital parameters throughout the operation.
4. Real-time imaging and navigation benefits
Advanced imaging technology plays an important role in modern laparoscopic surgery. High-definition camera systems provide surgeons with exceptionally clear images and can magnify the surgical field up to ten times the normal size. This enhanced visualization allows surgeons to detect subtle anatomical details that may be difficult to see in traditional open surgery.
Some advanced surgical systems provide three-dimensional imaging, which creates natural depth perception and improves surgical precision. This technology can be particularly useful during complex minimally invasive surgery procedures.
Certain imaging platforms also include fluorescence imaging, which highlights specific tissues or blood vessels to improve identification during surgery. In addition, computer-assisted navigation systems can overlay imaging data onto live video, giving surgeons additional anatomical guidance while performing delicate procedures.
These systems also allow surgeons to capture images and record important procedural steps. This documentation supports surgical quality monitoring and helps communicate important findings to your primary care physician following the advanced surgical treatment.